Can Mouth Guards Make TMJ Worse?
23rd May 2021

Mouth guards are a very common treatment for temporomandibular joint disorder (TMD), but can mouth guards make TMJ worse? TMD is a condition that affects the jaw joint, which is often referred to as the temporomandibular joint (TMJ). People with TMD often experience face and neck pain, jaw popping, headaches, and jaw pain. They might also clench their teeth or experience bruxism (teeth grinding), as studies have found the conditions to be related. Strain and direct injury to the jaw joint are often thought to cause TMD, though stress is also a factor. Sleep disorders such as snoring and sleep apnea have also been found to be related to TMJ symptoms.
The recommended treatment for TMD is often a mouth guard (sometimes called a splint or bite guard) because it can help relieve the strain placed on the jaw. Dentists might also recommend a night guard if your TMD is thought to be caused by bruxism.
It’s only natural to question new dental appliances and how they will affect your TMJ. Understand that your dentist is recommending a mouth guard because he or she believes it is the best option to treat your TMD, so the goal is for the oral appliance to make the condition better, not worse.

Can a Mouth Guard Make TMJ Worse?
In general, mouth guards should help—not hurt—TMD. However, not every mouth guard is right for every person or situation. The decision on which to use, when to use it, and how long to use it should only be made after a physical exam and open communication with your dentist.
To avoid a mouth guard or night guard making TMJ worse, it’s important to select the best oral appliance for your TMJ problems. When you take the proper steps: research your options, communicate with your dentist, and choose a high-quality custom-fitted night guard, your TMJ pain should subside.
If someone were to skip all the steps above and simply begin to wear any mouth guard, it is possible for the appliance to make their condition worse. TMD is a complicated disorder, and symptoms can be quite unique and vary from person to person. What works for someone else might not work for you. For this reason, it is important to have open discussions with your dentist about your TMJ symptoms.
Once you and your dentist decide which type of mouth guard to try, he or she should continually monitor you and check on your symptoms. TMJ should not worsen if you have regular oversight from your dentist because they will be able to identify problems in the treatment plan. You may need to try more than one treatment option to get it right, and that might even mean changing mouth guard types.
Karyn Kahn, DDS, a dentist at the Cleveland Clinic, explains “If the mouthguard doesn’t provide a comfortable bite, then the muscles won’t respond well, resulting in even more pain… With custom mouthguards, we can establish a comfortable relationship between your bite, your TMJ and the muscles that move your jaw” (2021). When you work closely with your dentist and use a custom-fit mouth guard, you will likely be able to find a solution that improves your TMD symptoms.
A meta-analysis that chronicled the efficacy of splint therapy for TMD found that mouth guards:
- Increased maximal mouth opening
- Reduced pain intensity
- Reduced the frequency of painful clicking episodes
Armed with the knowledge that a mouth guard can improve your TMJ pain, you can have an informed discussion with your dentist to find the best type of mouthguard for your condition.

Types of Mouth Guards for TMJ
Mouth guards are one of the most common forms of treatment for TMJ pain. The three most common types of mouth guards for TMJ are stabilization splints, repositioning splints, and NTI-tss devices.
Stabilization splints
Stabilization splints are often referred to as permissive splints, and they provide a barrier between the teeth by covering all upper and lower teeth surfaces. This type of oral appliance encourages wearers to leave their jaw relaxed and open, which helps the muscles relax.
Repositioning splints
Repositioning splints do exactly what their name suggests: they help reposition your lower jaw via indentations that do not allow teeth to slide freely. This type of splint is effective for people who have TMJ pain related to disc displacement (Pihut et al 2018).
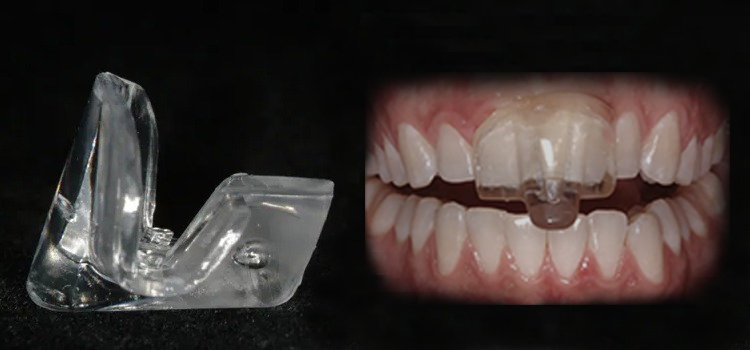
NTI-tss Devices
NTI night guards are designed to help people who are clenchers and grinders, because these repeated actions can contribute to TMJ pain. This device is worn only on the top front teeth.
When looking for and ultimately choosing a splint, it’s essential that you work with your dentist and choose a custom-fit mouth guard. Over-the-counter one-size-fits-all mouth guards are tempting because they’re cheap and easily accessible, but they can potentially cause further damage and pain. A custom night guard that is perfectly designed to fit your teeth is a safer option and is more likely to provide relief.
Related Articles:
- Best Mouth Guard For TMJ
- How Long Does It Take For A Mouth Guard To Work For TMJ?
- Teeth Grinding Headaches

How Mouth Guards for TMJ Work
As explained above, different mouth guards for TMJ work in different ways to alleviate pain and other symptoms associated with TMD. Mouth guards also help to prevent the teeth clenching and grinding known as Bruxism. Mouth guards can:
- Prevent teeth from grinding and clenching
- Reposition the jaw into proper alignment
- Encourage facial muscles to relax.
When mouth guards are chosen, fitted, and worn appropriately, they can:
- Alleviate facial pain
- Reduce jaw pain and soreness
- Protect the upper and lower teeth from damage and wear
- Alleviate headaches
Of course, a mouth guard for TMD will only work if worn as instructed by your dentist. Dental guards must be worn consistently for pain relief. You might also be wondering if a night guard for bruxism will help your TMD symptoms. While TMJ and bruxism do share some of the same signs and symptoms, the night guard you select should reflect your specific condition, which might require a mouth guard specifically tailored for TMJ. If your dentist has recommended a stabilization splint, repositioning splint, or NTI-tss device, it’s because he or she believes that will best solve your problem. Talk to your dentist about why a night guard for bruxism may or may not work in your situation. Ultimately, you and your dentist should work together to ensure you wake up each morning without chronic TMJ pain.
Alternative Treatments for TMJ Disorder
For various reasons, some people simply don’t want to wear a mouth guard. Even though mouth guards are one of the most popular TMJ treatments, there are many other effective treatment strategies you can try.
- Physical therapy: A 2020 retrospective review found that physical therapy reduced pain and increased maximal mouth opening in patients with TMD (Fisch et al 2020).
- Stress management techniques: Because both stress and anxiety can be contributing factors to TMD, finding effective management techniques can be helpful. This might include relaxation techniques or cognitive behavioral therapy.
- Botox: Botox can help relieve tension in your jaw muscles, reduce headaches, and reduce instances of lockjaw. A 2003 study found that over 90% of TMD patients who received Botox experienced reduced pain (Lindern et al 2003).
- Hot and cold therapy: A combination of ice and heat can reduce swelling, pain, and muscle tension. Try alternating heat and ice applied to the jaw a few times per day to relieve symptoms.
- Eating soft foods: Softer foods put less stress on the jaw muscles, and many people even find it difficult to eat hard foods when their TMD is flaring. Eating soft foods can give the jaw muscles a break and therefore help reduce inflammation.
Your dentist and other healthcare providers may have other treatments to suggest as well. He or she might prescribe a muscle relaxant or suggest surgical options for severe cases of TMD.
Related Articles:
Final Thoughts
TMD can have a direct negative impact on virtually every aspect of your life, from sleeping to eating to talking. Finding effective ways to manage your pain and other symptoms is essential to living a happy and healthy life. While treatments are important, you want to ensure anything you try will actually help your TMJ, not make it worse.
By speaking to your dentist and choosing a custom-fit mouth guard for TMD, you can reduce the likelihood that a mouth guard will make your TMD pain worse. Your dentist can help relieve your pain and avoid restorative dentistry by using a mouth guard and/or other therapies.
If you are experiencing TMD symptoms, you must take care of your oral health and make an appointment to visit your dentist. Trying to diagnose yourself and buying an over-the-counter TMJ mouth guard can actually make the problem worse.
References:
- Cleveland Clinic Writers. (2021). Should You Use a Dental Mouthguard for Your Jaw Pain? Health Essentials from Cleveland Clinic. https://health.clevelandclinic.org/should-you-use-a-dental-mouthguard-for-your-jaw-pain/
- Fernandes, Giovana, Siqueira, José Tadeu Tesseroli de, Gonçalves, Daniela Aparecida de Godoi, & Camparis, Cinara Maria. (2014). Association between painful temporomandibular disorders, sleep bruxism and tinnitus. Brazilian Oral Research, 28(1), 1-7. Epub May 09, 2014.https://doi.org/10.1590/1807-3107BOR-2014.vol28.0003
- Fisch, G., Finke, A., Ragonese, J., Dugas, L., & Wrzosek, M. (2021). Outcomes of physical therapy in patients with temporomandibular disorder: a retrospective review. The British journal of oral & maxillofacial surgery, 59(2), 145–150. DOI: 10.1016/j.bjoms.2020.08.068
- Pihut, M., Gorecka, M., Ceranowicz, P., & Wieckiewicz, M. (2018). The Efficiency of Anterior Repositioning Splints in the Management of Pain Related to Temporomandibular Joint Disc Displacement with Reduction. Hindawi: Pain of Temporomandibular Disorders: From Etiology to Management. https://doi.org/10.1155/2018/9089286
- Scaccia, Annamarya. (2018). Does Botox Help Treat Temporomandibular Joint (TMJ) Disorders? Healthline. https://www.healthline.com/health/botox-for-tmj
- Von Lindern, J. J., Niederhagen, B., Bergé, S., & Appel, T. (2003). Type A botulinum toxin in the treatment of chronic facial pain associated with masticatory hyperactivity. Journal of oral and maxillofacial surgery : official journal of the American Association of Oral and Maxillofacial Surgeons, 61(7), 774–778. DOI: 10.1016/s0278-2391(03)00153-8
- Zhang, C., Wu, J. Y., Deng, D. L., He, B. Y., Tao, Y., Niu, Y. M., & Deng, M. H. (2016). Efficacy of splint therapy for the management of temporomandibular disorders: a meta-analysis. Oncotarget, 7(51), 84043–84053. DOI: 10.18632/oncotarget.13059
- Most Popular
- Hard Outside, Soft Inside
- 2MM Thick
- Moderate / Heavy

- Most Durable
- Hard Materials
- 1.5MM Thick
- Heavy / Severe
- For Day Time Use
- Thin, Barely Visible
- 1MM Thick
- Light / Moderate

- For Clenching
- Flexible & Soft
- 1.5MM Thick
- Light / Moderate

