Good oral health not only protects the integrity of your teeth and gums but also ensures that your smile remains bright for years to come. Even if you brush and floss regularly, however, there are still some oral health concerns that you may end up facing. Whether a result of your lifestyle or your genetic endowment, these issues may be worrying and unpleasant, but they can all be addressed and managed.
Inside Your Teeth
To understand the problems you may face with your teeth, it is important to first understand what your teeth are made of. At the very centre of the tooth lies a cavity filled with nerves, blood vessels and other soft tissues. This is called the dental pulp. Surrounding the dental pulp is surrounded a hard yellowish material called dentin. Covering the dentin below the level of the gums is a layer of hard tissue called cementum, while above the gum line the dentin is covered by the hard, smooth, white outer layer of the tooth: the enamel. Each tooth sits in a space in the jaw bone supported by ligaments and surrounded by the soft gingiva or gum tissue.
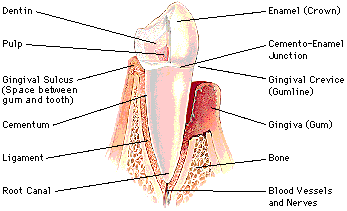
Each part of the tooth is vital to good dental health and a problem with any one part will usually lead to trouble for other parts of the tooth.
Bad Breath
Bad breath or halitosis can be a very embarrassing and concerning condition. Though bad breath can occasionally be the result of more serious non-dental conditions such as:
- Diabetes mellitus (acetone scent)
- Kidney failure (fishy smell)
- Liver failure
- Metabolic disorders (fishy smell)
- Lung or sinus infections
More frequently, however, halitosis is a side effect of other dental conditions. The smell itself is usually produced by the bacteria cells in plaque which produce odorous sulfur compounds. Since the tongue is very rough, it can be a site of food and bacteria accumulation. This collection of bacteria and its fuel--food debris--can result in large outputs of sulfur compounds which drive bad breath.
Bad breath can also be be caused by oral infection, cracks or chips in the teeth that gather extra bacteria, as well as periodontitis which can create hard to reach homes for sulfur producing bacteria. Fortunately, all of these conditions are treatable and halitosis has a high treatment success rate.
After you have confirmed with a doctor that there is not a more serious internal cause for your bad breath, a visit to your dentist is the next step. Your dentist can test the severity of your bad breath issue before treating any oral infections, cavities, and periodontitis. Your dental hygienist can then help you develop an effective oral health program (including specialized toothpastes and mouth rinses) that will help reduce oral bacteria and prevent recurrence of your halitosis problem.
Dry Mouth
Dry mouth is associated with a wide range of symptoms and causes and can lead to an increase in gingivitis, periodontitis, cavities, and other forms of oral disease. Fortunately, dry mouth (xerostomia) can be managed.
Signs of dry mouth include:
- Frequent thirst
- Impaired taste
- Difficulty speaking
- Dry burning sensation on the surfaces of the mouth
- Difficulty eating (dry foods)
- Difficulty wearing dentures
- Dry lips, cracking lips and corners of the mouth
These symptoms can be the result of natural aging, rheumatoid conditions, immune conditions, hormonal disorders, neurological disorders, longterm use of liquid and soft diets, radiation therapy, and any number of pharmaceuticals including decongestants, diuretics, antidepressants and a variety of others.
Unfortunately there is no straightforward cure for dry mouth but there are treatment options. The easiest way to reduce dry mouth is by drinking more water and keeping water with you throughout the day and night. Whenever you feel any dryness, just take a sip. Chewing sugarless gum can also help stimulate the salivary glands, while avoiding tobacco, alcohol, and sugary foods helps to prevent dryness. In some cases, using a saliva substitute (found in most pharmacies) may be the best treatment, allowing you to adjust your saliva levels artificially.
While treating dry mouth, it is also important to remember that the reduction in saliva (your body's natural oral rinse) can lead to increased plaque deposits, gum disease, and cavities. Thus, your oral hygiene plan deserves additional attention, and it becomes even more critical to use fluoridated toothpaste to protect your teeth.
Tooth Sensitivity
If eating ice-cream or drinking a hot latte is a source of agony to you, you may have tooth sensitivity. When teeth are damaged by physical trauma, teeth grinding, or cavities, or when the gums begin to recede in association with gum damage, the sensitive dentin and root surfaces can be exposed. These surfaces, when they come in contact with extreme temperatures, large differences in acidity, or even sugar, can cause sudden, intense, shooting pain in the teeth and jaws.
Chronic teeth grinding (bruxism), a lost crown or filling, cracked or chipped teeth, aggressive tooth brushing, gum disease, and periodontitis induced gum recession are the primary causes of tooth sensitivity. Unfortunately, with the exception of replacing a lost filling, most of these conditions are not reversible, but a good system of oral care can help reduce tooth sensitivity despite the exposure of sensitive surfaces.
In the case of severe sensitivity, dentists may use white fillings, fluoride varnish, or dentin sealer to cover the exposed root or dentin. If, however, you do not wish to undergo such procedures, there are some simple at-home solutions as well. First and foremost, you should maintain good oral health and hygiene using fluoridated rinses or toothpastes and a soft bristled toothbrush which will prevent further gum abrasions. Avoiding acidic foods which can erode enamel over time can also help prevent an increase in sensitivity.
Finally, there are many desensitizing toothpastes on the market which can actively reduce sensitivity. You many even want to spread a thin layer on the exposed roots and leaving it overnight. You may also need to try several different brands before you find the one that's right for you, but once you find one that works, you must keep using it or risk a return in sensitivity. The toothpaste is not curing your tooth sensitivity, it is merely managing it.
If your tooth sensitivity is connected to bruxism or tooth grinding, wearing a night mouth guard will prevent further erosion of tooth enamel, thus preventing an increase in sensitivity.
Gingivitis and Peridontitis
Healthy gums are usually light pink or coral, composed of firm orange peel textured tissues, and fitted closely to the teeth, following their contours and forming a scalloped edge. In this healthy state, gums will not bleed or cause discomfort during your daily oral hygiene routine, and there will be no visible redness or swelling. When plaque or tartar is allowed to accumulate along the gum line, however, these healthy tissues can become inflamed and painful. This development is called gingivitis.
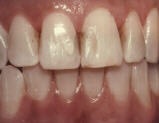
Gingivitis is usually indicated by red, swollen gums and bleeding during flowing and brushing. It is at this point that oral hygiene intervention can completely reverse the damage, but continued neglect can lead to the development of periodontitis. At the gingivitis stage, the gums are irritated, but the bone beneath them has not started to erode and there is no real lasting damage.
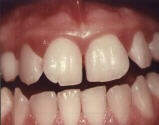
Once gum disease progresses to periodontitis, treatment is vital, but a full reversal of symptoms may be impossible as the bone around the teeth begins to degrade. In addition to the inflammation and bleeding seen in gingivitis, warning signs of periodontitis include:
- Gums pulling away from teeth
- Infection and pus around the teeth and gums
- Loose or separating permanent teeth
- Changes in your bite or the fit of a partial denture
- Bad breath
- Itchiness
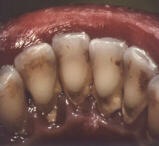
In the first stages of periodontitis, plaque and tartar appears below the gum line, the ligaments around the teeth degrade and the gums begin to separate from the teeth leaving a gap for more plaque and tartar to form. At this stage, professional plaque removal (scaling) and an active improvement in oral hygiene practices can prevent further degradation and maintain healthy gums and teeth. Unfortunately, the ligament structure will not recover and the teeth will always be more vulnerable to gum diseases.
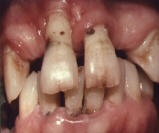
At later stages of periodontal disease, the ligaments have broken down, and the bone surrounding the teeth begins to degrade as well, pulling the gums far from the teeth. At this point, tooth sensitivity is common and swelling is severe. If left untreated, the condition may progress to the point that teeth are no longer fully supported in the mouth and must be removed to protect your overall oral health.
Regular visits to your dental hygienist and frequent self-checks can help catch and treat gum disease before it reaches irreversible levels. The best way to protect your gum health, however, is the maintenance of an effective oral health plan including regular brushing and flossing, use of a fluoridated toothpaste, and in some cases use of specialized mouth rinses.
Pregnancy Gingivitis
Starting in the second month of pregnancy and continuing for as many as six months after delivery, many pregnant women experience a sudden increase in gum swelling and redness. The hormones involved in pregnancy make the body more sensitive to the irritation of plaque near the gums. If, however, the plaque is removed regularly, the increased sensitivity will not lead to gingivitis all on its own. Just as with non-pregnancy gingivitis, the best prevention (and cure) is good oral hygiene. If you are concerned about the effectiveness of your oral hygiene routine, it's always a good idea to visit a dental hygienist and get professional advice.
Cavities
In addition to gum health, good oral hygiene can help prevent tooth damage in the form of cavities. When bacteria are allowed to remain on your teeth over time, particularly in the spaces between teeth, their chemical output gradually eats away at the tooth enamel. Low salivary flow, consumption of sticky sugary foods, and large gaps between eating sugary foods and cleaning the teeth, can all increase the likelihood of cavity formation. The natural strength, shape, and positioning of your teeth may also affect your risk of cavities.
Especially if you have a family history of weak enamel and frequent cavities, oral hygiene products containing fluoride will help to strengthen the tooth, harden your enamel, and even rebuild the tooth at the early stages of cavity formation. In combination with reducing problem foods such as candy and sticky starches like chips, and ensuring regular plaque removal, fluoride can help you maintain healthy cavity free teeth.
Tooth Grinding
Even with excellent oral hygiene, you may still face other dental concerns. Affecting 8-20% of the adult population (Lavigne et al., 2008), bruxism or teeth grinding can lead to a range of problems including tooth sensitivity, jaw pain, enamel erosion, and even the cracking and chipping of teeth. Most severe teeth grinding occurs during sleep and so can be very hard to diagnose until it reaches such severity that your partner can hear you grinding, or that you begin to suffer from pain, migraines, and visible tooth degradation.
The cause of bruxism is still unclear but stress seems to play a role in the severity and frequency of episodes. Thus, stress reduction and behavioural change therapies may be helpful in reducing the impact of bruxism. Ultimately, however, there is no certain cure so most dentists will recommend the use of a custom dental night guard. These guards fit closely to your teeth and protect them from the erosion and pressure resulting from grinding. Though they may be prohibitively expensive when purchased through a dentist, custom mouth guards can also be purchased safely and less expensively through online dental clinics such as proteethguard.com. No matter the cost, a mouth guard can reduce painful bruxism symptoms and protect your precious and irreplaceable tooth enamel.
Sports and Mouthguards
Physical trauma through sporting activities can not only lead to bruises and broken bones, but can also cause dental injuries which are unsightly, painful, and expensive to repair. In any contact sport, a mouthguard and a helmet should be worn as default.

Mouth guards for sport come in a variety of forms from the often large and clumsy (but cheapest) stock mouthguard, to boil and bite guards which allow a better fit through softening and moulding to the teeth, and finally to custom mouth guards fitted precisely to your unique bite by dentists or online dental clinics. A custom mouth guard will offer the best fit and protection without inhibiting breathing or speech, but they do tend to be more expensive than other options. Regardless of cost, the most important features of a mouth guard are:
- Complete and durable protection for all your teeth
- A good fit which ensures the guard won't fall out if you get hit
- No interference with breathing or speaking
- Comfortable
Once you've chosen a mouth guard that works for you, you can extend its lifespan by rinsing it in cold water after each use, occasionally cleaning it with soap and water, storing the guard in a closed container filled with water, and carefully watching for any signs of tearing or damage. As soon as you identify damage on the guard, it's time to replace it to ensure the best protection of your teeth.
Orthodontics (Braces)
In the quest for the perfect smile, many people choose orthodontics or braces to correct their tooth alignment and bite. Though typically chosen for aesthetic reasons, braces can also help to treat or prevent impaired chewing, speech problems, abnormal facial muscle function and swallowing patterns, and susceptibility to cavities, all of which are associated with misaligned teeth and bite patterns.
Because orthodontics work gradually, you may have to wear them for several years. Your dentist may be able to fit you with clear or white braces rather than the traditional silver apparatus, but if you are choosing to wear braces, your dental hygiene become more important than ever. Braces leave lots of hard to reach places that can collect food and plaque, so it is best for orthodontics wearers to brush after every meal and make use of smaller interdental brushes to reach around and behind the wires and bands of the braces. Mouth rinses and special flossing tools can also help remove plaque and food debris. Additionally, wearers should avoid sticky or hard to chew foods that can not only stick in the teeth and lead to cavities, but which may also stick to and bend or break the wires of the braces.
Orthodontic appliances like braces can do a lot to improve your smile, but they also increase the risk of plaque and tartar build-up. If you are going to be wearing braces, especially over a long period of time, you will need to be extra diligent in your oral hygiene practices.

Dentures
If you wear dentures, it is important that they fit well so that you can eat and talk comfortably and that they are kept clean to prevent gum damage, mouth odour, and irritation or infection. To maintain clean, comfortable, stain free teeth you should rinse the denture under water after every meal, brush the denture with water and denture paste (or a mildly abrasive toothpaste) at least before bed but ideally after every meal, and soak the denture daily in a denture solvent such as Efferent or Polident.
When cleaning your denture it is important to work lightly with a soft brush to prevent scratching or breaking--never use sharp tools to scrape off deposits, take it to your dentist for cleaning instead. You may want to work over a sink filled with water and with a towel in the bottom to cushion the denture if it is dropped. While cleaning, it is also important to avoid hot water and to always submerge the appliance in cool water when it is out of your mouth. Both of these practices protect the fit of the denture.
Even maintaining the original fit of your denture, the shape of your jaw changes with age so you may end up with ill-fitting dentures no matter how well you care for them. In you are noticing problems chewing or speaking, redness and inflammation in your mouth, discomfort, cracks around the corners of your mouth or chronic cheek biting, it may be time to return to your dental professional and arrange a refitting.
While you are wearing dentures, you must also be sure to give your gums the care that they deserve. Dentures should be taken out overnight or left out of the mouth for 6-8 hours each day allowing your gums to breathe. Your gums will also require daily cleaning with a soft toothbrush or cloth to remove debris and stimulate blood flow. You can further massage your gums using your thumb and index finger to lightly press and stroke the ridge of the gum. Like your gums, any remaining natural teeth also require care. Brush and floss them regularly and thoroughly and you may be able to extend their lives significantly.
Tooth Bleaching
In our image obsessed society, it is easy to feel self-conscious about your teeth if they are stained or yellowed. These stains can be internal as a result of injury to the tooth or certain medications, or external as a result of food and drink or smoking habits. Internal stains are very difficult to remove and even bleaching may not get rid of them. External stains, however, are receptive to bleaching and can be removed and prevented by good oral hygiene habits.
In order to determine what sort of stains you are facing and whether or not profession or home bleaching is right for you, you may wish to visit your dentist or dental hygienist. Dental professionals can help you reach your whiteness goals without damaging your teeth or gums with careless or overzealous bleaching. If you decide to bleach at home, be sure to follow all instructions carefully and contact your dental professional if you experience any lasting or severe side-effects.
Smoking and Oral Health
Smoking and other tobacco use is not only damaging to your lungs, but also causes a diversity of oral health concerns. Some of the potential problems are:
- Tar deposits and staining of teeth
- Inflamed roof of mouth and palate
- Delayed gum healing
- Increased gum disease
- Bad breath
- Black hairy tongue
- Oral lesions
- Gum recession
- Oral cancer
The most severe of these effects is oral cancer which in 75% of cases is directly associated with tobacco and alcohol use. Your risk of all of these symptoms can however be reduced by tobacco use cessation. Even after years of smoking, within 10 years of not smoking, oral cancer risks return to normal levels. There are many stop-smoking aids available from nicotine gum and patches to support groups and aversive therapy. If you are ready to stop using nicotine, a dental or health professional can help you choose an effective way to quit.
Oral Cancer
Like skin cancer, if oral cancers are caught early, they can often be removed with limited damage to your overall health. Because your dentist can't check your mouth everyday, you may want to begin performing self-checks. Be aware of the appearance and feel of your oral cavity and be particularly conscious or any swellings, lumps, or growths in the mouth or neck, discoloured patches in the mouth, repeated bleeding from the mouth or throat, and any difficulty in chewing or swallowing. If you have any concerning signs or any sore that doesn't heal within two weeks, you should visit your dentist or physician to have the sore or growth checked and biopsied as needed.
To perform a full oral cancer self check you will need to:
- Examine your head and neck visually looking for any sores, moles, discolouration, or asymmetry
- Press the skin along your neck feeling for any tenderness or bumps
- Visually examine the inside of your lips for discolouration or sores
- Run your thumb and forefinger along your lips pressing and feeling for any lumps or tenderness
- Visually examine the inside of your cheek, pulling it outwards with your fingers
- Press and feel along the cheek for any bumps
- Tilt your head back with a wide open mouth and look for any lumps or sores on the roof of your mouth
- Stick out your tongue and visually examine all surfaces of the tongue for sores or discolouration
- Press and feel along the underside of the tongue for bumps or swelling.
If you have any concerns it is always better to see a health professional and have it checked.
Get Started with Healthy Teeth and Gums
A healthy mouth is vital for comfortable eating and speaking, and for maintaining good self-esteem. Though there are many potential oral health concerns, most of them can be prevented or managed by good consistent oral hygiene practices such as twice-daily brushing with fluoride toothpaste and regular flossing. Dental professionals can treat oral health issues and can help you set up good oral health habits, but ultimately prevention starts with you making good choices in food and drink consumption and dental care.
References
Lavigne, G.J., Khoury, S., Abe, S., Yamaguchi, Y., Raphael, K. (2008). Bruxism physiology and pahtology: An overview for clinicians. Journal of Oral Rehabilitation, 35, 476-494.